Emergency/911 operators in Phoenix, Arizona recently received a shocking call from a local long-term care nursing facility. The nurse on the other end of the line was frantic. It was January 11, and a patient at the nursing home had just given birth to a baby boy – the child was not breathing. “The baby’s turning blue. We need someone now!” the caller shouted. “We had no idea she was pregnant. We were not prepared for it.” [1]
The nurse was given instructions in infant CPR and the baby began crying shortly after. The child is now in good health and is in the care of his mother’s extended family. However, several disturbing questions were raised by the incident. First, the woman in question had been in a largely vegetative state in this facility since a near-drowning at the age of three. Who had access to this woman and had assaulted her while under the purported care of the nursing facility? Also, she delivered a full-term baby, meaning that she had been pregnant for roughly nine months. How had her doctors not noticed her condition?
An investigation was launched shortly after the birth of the child, and a few weeks later an arrest was made. The apparent father of the child is a man named Nathan Sutherland, who was a nurse partially responsible for care of the woman. DNA samples were taken from all employees at the nursing home, and his sample matched that of the child. [2]
Repercussions from this incident have since spread beyond the rapist. The CEO of the nursing facility resigned following the scandal, and both doctors who attended to the patient are no longer working there (one resigned, and another was suspended). [3] The owner of the facility has hired a former county attorney to lead an internal investigation into the incident. He will investigate security surrounding the facility, examining issues including visitor admittance, security guards, and the placement of surveillance cameras.
While this story is particularly shocking, abuse in long-term care facilities is not uncommon. A factor in this case that was perhaps most unusual was the age of the patient. Most individuals in long-term care facilities are elderly. Age weathers people and leaves many unable to care for themselves without help of family or hired help. Many elderly individuals are forced into nursing homes out of necessity, where there is little oversight to prevent abuse and neglect.
Elder abuse is becoming a more serious issue nationally because the percentage of the U.S. population that is advanced in age is increasing steadily. The two segments of the U.S. population that are currently increasing in size are the group in the 1-18 age range and those over the age of 60. In comparison, the percentage of the U.S. population between the ages of 19-59 is decreasing. This is doubly concerning, because it is the middle demographic that we would expect to be caring for those in the 60+ segment.
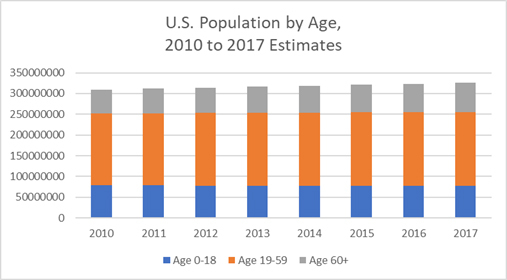
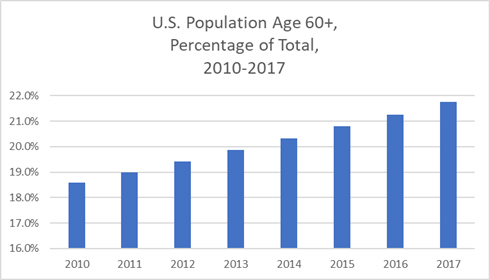
The percentage of the U.S. population that is elderly has risen from 18.5% in 2010 to over 21% in 2017. One could attribute this increase to a number of factors. The birth rate has fallen in recent decades due to easier access to contraception and women tending to wait longer to start families, in part because social change has made it easier for women to break into and ascend in professional careers once largely closed to them. Medical care for the elderly has also improved, leading to longer lives for many. Part of the issue is also purely demographic – the large cohort of so-called Baby Boomers, born between 1945 and 1965, have been reaching old age in recent years. Whatever the cause, what we know for certain is that the number of individuals who need intense, live-in care due to their age is rising steadily, while the number of people able to provide that care, along with their financial and infrastructure resources, is remaining static. For a clearer understanding of the percentage increase in the U.S. population that is elderly and in possible need of long-term nursing facilities, see the chart below.
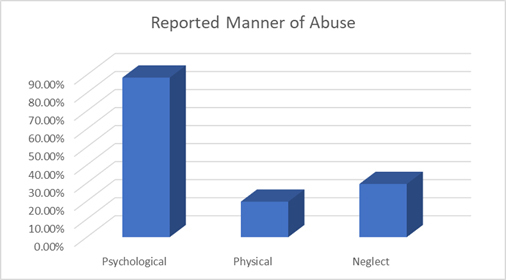
As one might expect, the confluence of a large, frail elderly population, along with fewer caregivers, often leads to cases of neglect and abuse. In 2010, a study found that 47% of study participants with dementia had been mistreated or abused by caregivers. Of those who had been treated poorly, 29.5% had experienced neglect, 19.7% had experienced physical abuse, and 88.5% had been subjected to psychological abuse. [4]
Nevada has taken steps to help reduce the likelihood of neglect and abuse in long-term care nursing facilities. The state attorney general’s office released a guide to help law enforcement officials recognize signs of elder abuse in order to help victims and prevent further abuse and neglect. The AG’s office also hopes to help victims of abuse access much-needed services. In order to meet this goal, it has earmarked additional grant money that will go toward direct services for elderly victims of abuse, including sexual abuse, domestic abuse, financial exploitation, and neglect. [5]
If you or a loved one is a victim of real or suspected abuse in a nursing facility, contact law enforcement immediately to report the issue. Reporting abuse can be instrumental in protecting an abused individual and preventing future victims. If you feel you have sustained injuries in relation to abuse or neglect in a long-term care facility, be sure to contact a personal injury attorney to understand your rights as an injured party.
[1] https://www.buzzfeednews.com/article/ellievhall/we-had-no-idea-she-was-pregnant-nursing-home-staff-t… [2] https://www.washingtonpost.com/nation/2019/01/24/nurse-accused-getting-patient-pregnant-was-christia… [3] https://www.telegraph.co.uk/news/2019/01/23/nurse-arrested-arizona-care-home-patient-pregnancy [4] https://ncea.acl.gov/whatwedo/research/statistics.html [5] https://mynews4.com/news/local/nevada-attorney-general-releases-guide-for-elder-abuse-neglect-invest…



